About AMR
What does AMR mean for veterinary practice?
When microorganisms become resistant, simple infections can become chronic, serious, or even life threatening.
This leads to increased costs of veterinary care, more antimicrobial use, and a higher rate of treatment failure. More antimicrobial use leads to more selection pressure for resistance and a growing reliance on a shrinking group of effective antibiotics.
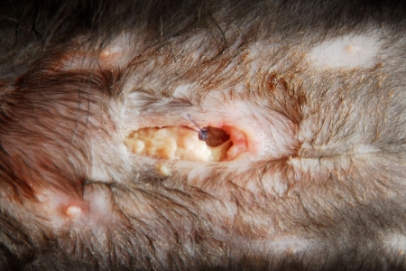
In veterinary practice today we are seeing an increase in resistant surgical site infections and simple urinary tract infections that cannot be treated with standard antimicrobial choices.
Reducing our use of antibiotics when they are not needed can help to ensure that these life savings medicines remain effective when we really do need them.
Current AMR examples

Food-producing animals and AMR
There is increasing focus on the risk of animals and their products as a source of resistant bacteria
entering the food chain, particularly in relation to common foodborne pathogens like Escherichia
coli,
Salmonella spp., Enterococcus spp., and Campylobacter spp.
Both the Australian and New Zealand government currently assesses the risk of AMR transmission to humans from domestic food-producing animals to be low. This is due to factors such as:
- Strict regulation on the registration of veterinary medical products. For example colistin, a high-priority critically important antibiotic (HP-CIA), is not registered for use in food producing animals in either Australia or New Zealand. Fluoroquinolones (classified as HP-CIA), are not registered for use in food-producing animals in Australia, however they are registered for use in pigs and cattle in New Zealand.
- Both Australia and New Zealand have a relatively high proportion of extensive farming systems, particularly in the red meat industries.
- As island nations free from a number of diseases that impact other continents, New Zealand and Australia have a strong focus on biosecurity, both at the farm and the national level.
- Using standardised measurements set by the European Medicines Agency, Australia and New Zealand report relatively low levels of antimicrobial use in food-producing animals.
Based on data from 2010-2012, a 2015 review on AMR by the British government ranked New Zealand as the third lowest user of antimicrobials in food producing animals, behind Norway and Iceland, compared with 26 European nations and the United States (New Zealand – approximately 9.4mg active/ kg biomass). Australia’s 2009/2010 use ranked fifth lowest in this review, reporting levels similar to Sweden at that time (approximately 20mg active/kg biomass).
In line with a directive from the World Health Organisation, the OIE, and the FAO, both Australia and New Zealand have created National Action Plans to address AMR which include optimising antimicrobial use in food-producing animals. Government and industry have been working together to implement these plans through initiatives such as the development of industry specific stewardship programs and antimicrobial prescribing guidelines.
Veterinarians in Australia and New Zealand have an important role to play in supporting clients to adapt their practices and production systems in order to support their country’s commitment to optimise antimicrobial use in food-animal production.
See the following links for further information:
European Medicine Authority report on AMU in the EU, 2018 report.
New Zealand govt gross usage report 2020 (based on 2018 sales).
APVMA Gross usage report from 2014 (based on 2005-2010 sales).

Rhodococcus equi in horses
Rhodococcus equi most commonly causes pyogranulomatous pneumonia in foals, colloquially known
as
‘Rattles’. As a soil saprophyte, R. equi can survive and persist on a property for a prolonged
period of
time, causing disease in foals in subsequent breeding seasons. The disease has traditionally been
treated with combination therapy of rifampicin and a macrolide antibiotic, but recent trends show an
increase in resistance to these agents.
To reduce the incidence of disease, some endemic properties practice blanket treatment of all foals. However, there is evidence that blanket treatment contributes to resistance, making the disease more and more difficult to manage over time. Most foals with clinical signs of rattles do require antimicrobial therapy, but subclinical and self-limiting cases also occur which do not require treatment.
On endemic properties, the use of targeted rather than blanket treatment combined with management practices to minimise exposure in foals is recommended best practice. Periodic monitoring of foals and the use of ultrasonographic scoring can identify those foals that do require treatment, reducing the overall use of antimicrobials and thus the selection pressure for resistance.
For further information see this controlled, randomized and double blinded field study conducted on a Warmblood stud in Germany which was affected by endemic seasonal pneumonia due to R. equi, Venner et al (2013).

MRSP in dogs
Staphylococcus pseudintermedius is a commensal bacterium of dogs, and is occasionally isolated
from
other companion animals, such as cats and horses. One of the greatest concerns in canine practice is the
rapid emergence of methicillin-resistant Staphylococcus pseudintermedius (MRSP).
Like its relative, methicillin-resistant Staphylococcus aureus (MRSA), MRSP is a coagulase-positive staph that is resistant to all ß-lactam antibiotics. However, MRSP is not the same as MRSA. Despite posing difficulties to veterinary practice, MRSP is infrequently a cause of disease in humans.
As a great opportunistic pathogen of dogs, MRSP is commonly associated with cystitis, skin disease, and surgical site infections (especially in cases where there is an indwelling implant).
Routine skin carriage of this organism is increasing in dogs throughout Australia. The extremely drug-resistant nature of MRSP poses a genuine threat to our ability to engage in routine procedures.
By invoking antimicrobial stewardship principles we can reduce the selection pressure driving the emergence and spread of MRSP.
For further information on MRSP in Australia see this retrospective study investigating all coagulase-positive staphylococcal isolates from Australian veterinary diagnostic laboratories during 2013, Saputra et al (2017).

Find out what the following organisations have to say about AMR:
Australia
Australian Government - Go to site
Australian Veterinary Association - Go to site
New Zealand
New Zealand Government - Go to site
New Zealand Veterinary Association - Go to site
Global
WOAH - Go to site
WHO - Go to site
FAO - Go to site

